Secondary Brain Injury: When Recovery Goes Off Track
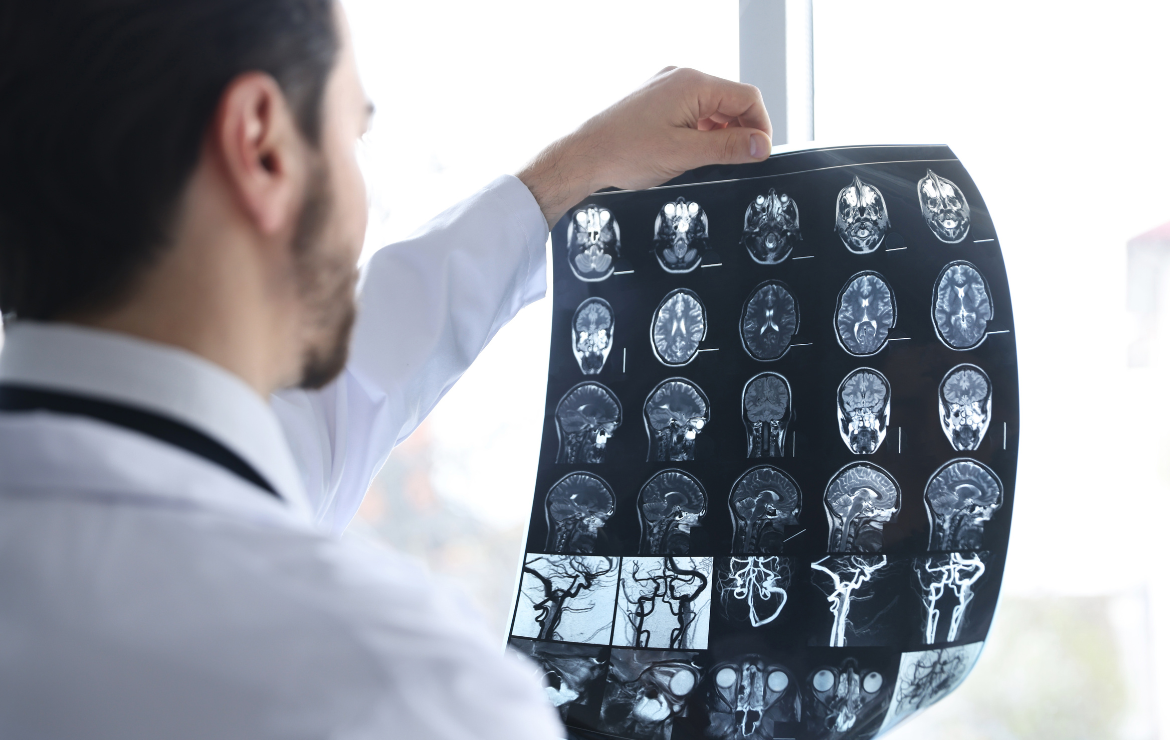
When most people think of a brain injury, they think about the moment of impact, such as a fall, a vehicle accident, or a blow to the head. That first event is called the primary injury. But sometimes what happens afterward causes just as much trouble. This is known as secondary brain injury, and it is one of the most overlooked reasons recovery can drift in workers’ compensation claims.
A primary brain injury is the immediate damage caused by trauma. A secondary brain injury develops after that initial event. It can involve swelling, reduced oxygen, inflammation, or chemical changes inside the brain. Think of it like a house fire. The first injury is the spark. The secondary injury is the smoke that continues to spread after the flames are out. In some cases, the smoke causes more damage than the original fire.
You may see a claim labeled as a mild concussion with normal imaging. On paper, it looks straightforward. But days later, the injured worker reports worsening headaches, difficulty concentrating, mood swings, or trouble sleeping. They may seem forgetful or overwhelmed. From the outside, it can look like poor effort or delayed recovery. From the inside, the brain may still be healing.
The brain has soft tissue inside a hard skull. When the head moves suddenly, the brain can shift or stretch. Even if scans look normal, irritation at the cellular level can still exist. If swelling increases or oxygen levels drop, symptoms may worsen. The injured worker may struggle to process instructions, tolerate noise, or manage normal work tasks. Recovery slows. Return to work becomes harder.
Sometimes brain injury is not even the main diagnosis. We see cases where the primary focus is orthopedic, such as a fracture or surgery, but the worker also struck their head. The claim centers on mobility and physical healing. Meanwhile, subtle cognitive symptoms go unrecognized. Months later, the worker misses appointments, misunderstands directions, or family members say they are not the same. That is often a signal to reassess.
Secondary effects are not always dramatic. Pain increases stress. Stress disrupts sleep. Poor sleep slows healing. Frustration builds. This cycle can quietly push recovery off track. I am not sure exactly how often this happens in workers’ compensation, but clinically we see enough to know it matters.
For adjusters and nurse case managers, awareness is key. You do not need to overreact to every symptom. But if recovery does not match expectations, pause and ask questions. Are cognitive symptoms documented? Was follow up recommended? Did the injured worker fully understand discharge instructions? Are transportation and language services properly arranged? Small gaps in coordination can create larger setbacks.
One of the biggest risks in complex claims is maintenance mode. Services continue and the claim feels stable. But stable does not always mean improving. Brain injuries, especially mild or secondary ones, can hide in quiet files.
We will explore this topic further in our upcoming Brain Recovery Management CEU, where we will break down how secondary brain injury develops, how to recognize subtle warning signs, and practical steps claims teams can take to keep recovery moving forward. Register Today for CEU
Brain injuries are not always visible. When something feels inconsistent with the expected recovery path, it is worth a closer look. Early recognition can make a meaningful difference for both the injured worker and the claim.